Quality of Life
Grant Recipient
2013 & 2015


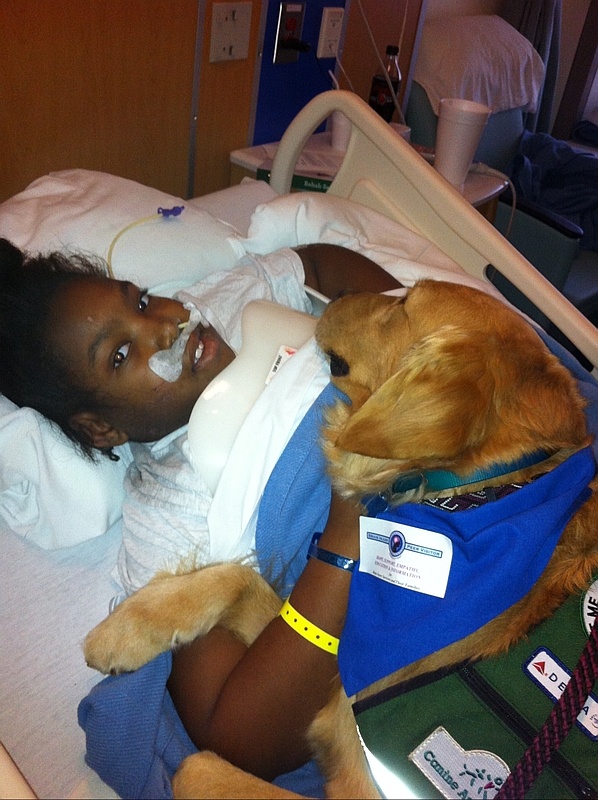
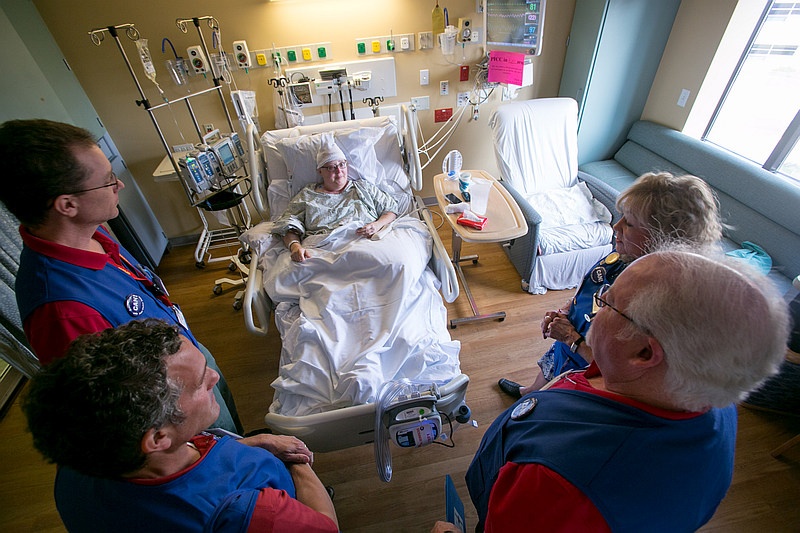
We offer Hope, Peer Support, Empathy, Education, and Information for hospitalized and rehabilitating brain injury survivors and their families.
We are a team of trained volunteers, including our director.
We provide face-to-face Peer Support Visits:
We visit with over 9,500 brain injury survivors and their caregivers each year.
Our Peer Visitor program is for ALL types of brain injuries, including:
- Aneurysms
- Anoxia
- Beatings
- Brain bleeds
- Brain diseases
- Car wrecks
- Cerebral Palsy
- Chiari Malformation
- Concussions
- Drug Overdose
- Falls
- Military service
- Sports injuries
- Strokes
- Surgery
- Tumors
- etc.
We are a 501(c)(3) non-profit organization¹.
The Brain Injury Peer Visitor Association team members give peer support and resources at a critical time in the recovery process.
A Role Model
For the survivor, family members, and friends, to see how recovery from brain injury can result in a happy and healthy life. We demonstrate how survivors learn to cope with their injury or illness, and learn to develop compensatory strategies and acceptance.
Direction
A “roadmap” which will assist caregivers and survivors in navigating the road ahead, including how to obtain financial support for therapies, treatments, and services from organizations that provide monetary support.
Empathy
A listening ear and a sounding board for caregivers and survivors.
Coping Strategies
Sharing positive strategies that have worked for each of us.
Information and Referral Services
- Brain injury
- Community resources
- Financial and governmental services
- Support groups
- State brain injury associations
- Stories from survivors
- Lists of books and websites
- How to care for someone with a brain injury
- And much more . . .
Watch this YouTube video about our association:
¹ A copy of this foundation’s annual return is available upon written request to Ann Boriskie (see Contact Us page).